Is Context King?
Posted on 26th January 2024 by Justin Martino

What are contextual factors?
Contextual factors in healthcare encompass the various factors outside of the intended targets of treatment (specific factors) or natural history and regression to the mean (non-specific factors), which can significantly influence a patient’s outcomes. The result of these is known as the “contextual effect” of any given treatment. Contextual effects are important for researchers and clinicians alike because they can significantly affect how patients respond to treatment– for better or worse. [1]
More specifically, the international consensus definition of contextual factors is as follows:
“Contextual factors (CFs) are components of all therapeutic encounters and may constitute the entirety of the perceived effects of the intervention itself or be additive to effects of interventions such as pharmacological and non-pharmacological treatments.
CFs are perceived cues that affect both the patient and practitioner and can arise from previous experiences and immediate dynamics within the encounter, or a combination of both. CFs fall into broad categories that can include patient characteristics, practitioner characteristics, treatment characteristics, characteristics of the dynamic between the patient and practitioner and characteristics of the setting within which the encounter is being delivered.
CFs can be complexly interwoven in the patients and practitioners experience so as to influence what patients and practitioners expect the outcome of the encounter to be. Through such conscious and unconscious expectations, involving a range of specific neurological pathways, CFs can directly influence (both positively and negatively) symptoms and characteristics associated with the presenting condition. The proportion of clinical effects observed associated with CFs can vary from large to small depending on the characteristics of the patient, practitioner, condition and intervention”. [2]
Disclaimer: Researchers often define contextual effects differently across studies by choosing either to include or exclude non-specific effects (regression to the mean and natural history) in their definition. However, I believe that for the context of research, it is important to disentangle contextual effects and non-specific effects, as this would better separate the modifiable and non-modifiable. By separating these two concepts, we can better understand what clinicians can do to make more of an impact on their patients.
So, is this just a placebo?
Again, that depends on who you ask within research. However, the Society for Interdisciplinary Placebo Studies differentiates between “placebo effects” and “placebo responses,” which a “placebo treatment” can be used to ascertain. Placebo effects are specific changes in a patient’s health that can be directly attributed to their body’s response to the belief in a treatment, sometimes brought on by a placebo treatment. [3] This is believed to occur primarily due to mechanisms of the central nervous system. Whereas the term “placebo response” encompasses all health changes observed after administering a placebo treatment, now including both placebo effects and non-specific effects (natural progression or regression to the mean). [4]
As such, I prefer to use “placebo effects” as opposed to “placebo response”, in research, as it is more akin to my preference of defining contextual effects without non-specific effects– making the research of placebo/contextual effects more actionable for clinicians because it isn’t so confounded by non-modifiable factors.
Nevertheless, natural history and regression to the mean are massively important for understanding treatment across diseases and disciplines in healthcare. With this being said, the crux of the argument between defining placebo effect and contextual effect then comes down to whether or not you consider the placebo effect as just being caused by the belief in treatment or if it’s caused by the entire context of the treatment; the prior implies a difference between placebo and contextual effects while the latter asserts them to be the same thing. Similar to contextual effects being defined differently across research studies, so too is the placebo effect– either being defined as different or the same as contextual effects based on the aforementioned statement. [4,5]
How do we investigate this in research?
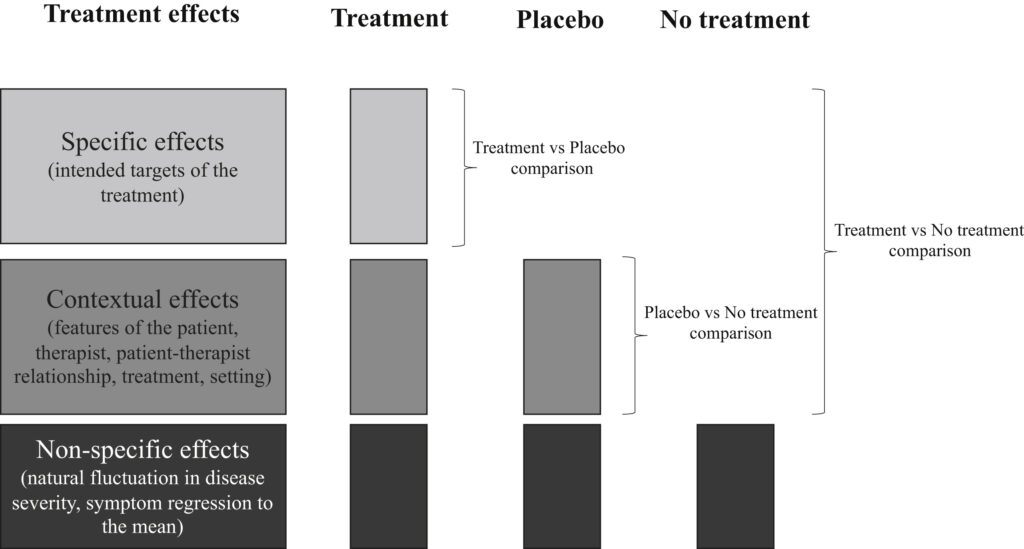
The total treatment effect of a given treatment is a combination of its specific effects, contextual effects, and the non-specific effects. Within research, we can disentangle each of these by having a 3-armed study, consisting of a treatment arm, control arm, and a no treatment arm. By using each of these we can determine what the treatment arm does that the control doesn’t (specific effects), what the control arm does that the no treatment doesn’t (contextual effects), and what the no treatment arm does in isolation (non-specific effects). [1]
Figure 1. How to disentangle specific effects, contextual effects, and non-specific effects (DOI: 10.1016/j.joca.2020.12.011; License: CC BY-NC-ND)
How much does this even matter?
Understanding contextual factors is important for healthcare workers as these factors significantly influence patient outcomes. Contextual and non-specific effects, when grouped together, have been indicated as most of the total treatment effect across healthcare. [3,6] But when disentangled and looking specifically at short-term pain relief for patients with chronic low back pain, 33% can be attributed to the specific effects of treatment, 18% to contextual effects, and 49% to non-specific effects. [7] By acknowledging this and trying to optimize these factors in clinic– by simultaneously fleshing this topic out in research– we can try to optimize patient outcomes across a variety of treatments and fields.
Conclusion
Contextual factors in healthcare encompass a range of elements which influence the outcomes of therapeutic encounters, extending beyond direct treatment effects. They play a crucial role in shaping both the perception and the actual impact of medical interventions, affecting outcomes either positively or negatively. These factors, often intertwined and complex, are key in determining how patients respond to both pharmacological and non-pharmacological treatments, and they contribute significantly to the overall effectiveness of healthcare, making their understanding and optimization crucial for improving patient outcomes.