Timing of hypertonic saline and airway clearance techniques in adults with Cystic Fibrosis during pulmonary exacerbation: a critical appraisal
Posted on 3rd June 2019 by Elizabeth McEneaney
This blog is a critical appraisal of the following randomized controlled trial: Timing of hypertonic saline and airway clearance techniques in adults with cystic fibrosis during pulmonary exacerbation.
Background
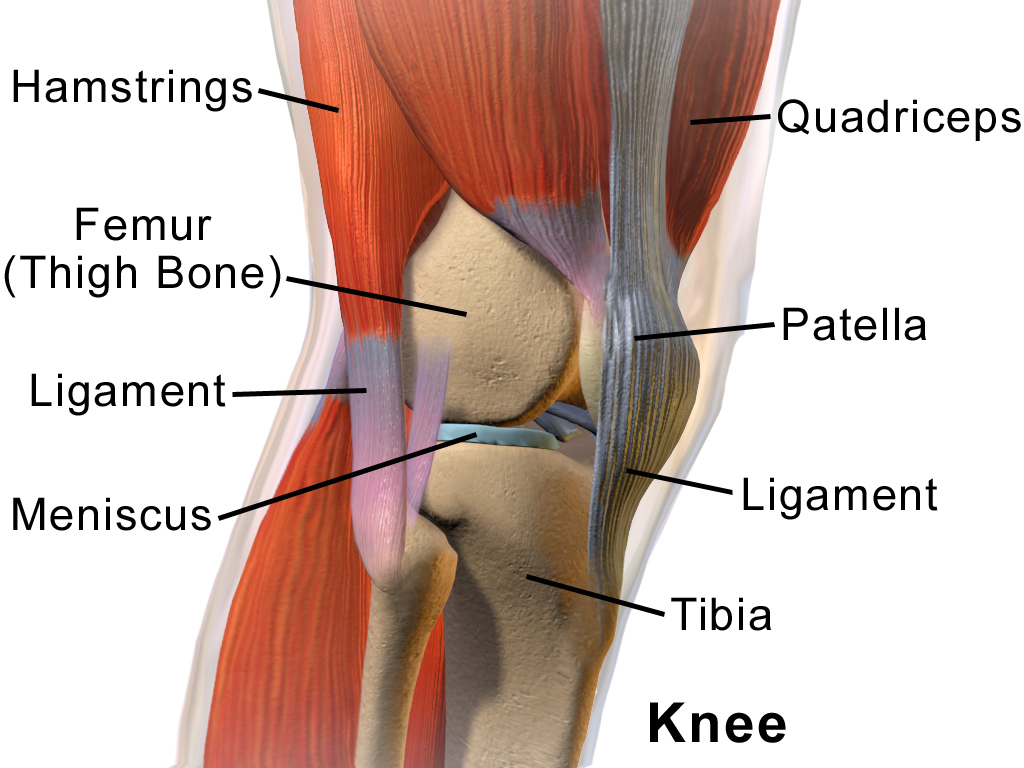
Cystic Fibrosis (CF) is a clinical condition affecting the CF transmembrane gene causing problems with chloride transport and impaired ciliary, therefore generating increased production of thick mucus, causing blockages within airways leading to serious lung infections (Port and Matfin, 2009). CF remains a life limiting condition, although advances in medical management have resulted in a delay in the decline of lung function and significant improvement in life expectancy. (NICE, 2015) There is clear evidence that airway clearance techniques (ACT), such as daily hypertonic saline (HTS) improve mucus clearance and reduce the frequency of exacerbations. Recent research strategy has shifted from examining the comparative efficacy of different ACTs to the study of ways to optimise the application of techniques.
What was the study?
This pilot study was designed to compare the change in Lung Clearance Index (LCI) ventilation distribution measure by multiple breath wash out (MWB) at 90 min post treatment with HTS inhalation before ACT compared with HTS inhalation during ACT in adult patients with CF. 14 subjects were recruited and 13 completed the study. Inclusion criteria entailed subjects with CF aged ≥18, near the end of a 10 – 14 day intravenous antibiotic (IVAB) therapy course for pulmonary exacerbation. Participants also needed to be productive of sputum ≥10g over 24 hours on enrolment and currently/previously used and tolerated HTS. Written consent was also required. Randomisation of participants was electronically generated and concealed by an administrator independent of the study. Treatment was assigned and carried out by a qualified respiratory physiotherapist. The assessor conducting the outcome measures was blinded to the treatment intervention order. The primary outcome measure was the LCI, due to its superior sensitivity. Secondary outcomes included change in FEV1% predicted, forced expiratory flow (FEF) predicted, 24 hour sputum volumes, patient/physiotherapist perceived ease of clearance and satisfaction with treatment, number of coughs and duration of treatment.
Results
Overall the LCI showed no significant difference, HTS before ACT – (MD(95% CI) 0.10, HTS during ACT (MD(95% CI) 0.12, yet functional residual capacity (FRC) was remarkably reduced with HTS during ACT (MD(95% CI) – 0.11 but was unchanged with HTS before ACT (MD(95% CI) 0.55. Secondary outcome measures also demonstrated no statistical significance. These findings were based on the 95% confidence intervals. The wide intervals presented in this study are due to statistical variations, which do not represent the larger population.
Strengths and weaknesses of the study
The use of a crossover trial was an appropriate design to address the question posed by this clinical trial. It removes bias, with each subject acting as their own controls, ensuring that all other participant criteria and potentials for difference in results remain the same. The target group of the study were currently inpatients receiving IVAB for an exacerbation in pulmonary symptoms. This was necessary as the trial was carried out over two consecutive days, which may not have been feasible in an outpatient setting. The study endeavoured to ensure that each trial participant had returned to their stable status. This recruitment process was as clearly defined as it appeared. Two subjects failed screening due to increased ill health, also the effects of pulmonary exacerbation on lung function cannot be dismissed, therefore, affecting accuracy of results. The sample size of the study was extremely small consisting of 13 participants, the enlisting criteria for the trial proved quite demanding. For data to be clinically relevant the findings need to be reproduced in a larger sample.
Attempting to minimise bias and improve internal validity, randomisation of participants was carried out via electronic generation and concealed by an administrator independent of the study, the assessor overseeing the outcome measures was also blinded to the treatment intervention. Due to the nature of the treatment the physiotherapist could not be blinded; this could possibly influence results.
The (MBW) test used to measure LCI relies on breathing out at normal tidal volumes. Researchers ensured it was carried out either before or at least 30 mins after spirometry measurement, so as to avoid any confounding effects of forced expiration on the expired volume during the washout phase.
LCI proved somewhat unpredictable as the FRC (the volume of air present in the lungs at the end of passive expiration) a component of the LCI tended to fluctuate after physiotherapy intervention, particularly when using HTS during ACT, as FRC had significantly decreased. This was possibly due to the opening of previously obstructed airways but there was no change in LCI. LCI measurement may not be as straightforward in those with significant airflow obstruction, which a large proportion of participants presented with.
Wet weight sputum was used as a secondary measure for convenience and the ability to measure quantity produced. However, wet weight sputum is increased due to saliva contribution, introducing error. Do we measure volume or weight?
Conclusion
The results from this pilot study could not support the hypothesis that HTS before ACT was more effective that HTS during ACT. However HTS during ACT resulted in a shorter treatment time, suggesting that if length of treatment time affects adherence, HTS during ACT offers an equally effective treatment but of a shorter duration. Further research needs to be conducted over a longer time period and with a bigger sample group.