Natural history and prognosis for musculoskeletal rehabilitation students
Posted on 31st January 2022 by Christopher Hughen

A diagnostic heavy curriculum
Within physical therapy education in the United States, there is a large emphasis on teaching students how to find a diagnosis. Was there a specific mechanism of injury? What patterns am I looking for? What objective testing do I perform? What ‘special tests’ should I implement? What are the pre- and post-test probabilities of performing said ‘special tests’? Are there well validated clinical prediction rules to guide my decision making? All of these questions are valuable and the ability to perform a thorough differential diagnosis is necessary.
Moving beyond a diagnosis
Now that I have come up with a potential working diagnosis, where do I go from here? How do I explain this condition or injury to my patient? How long will it take for them to get back to doing what they value? What interventions should I provide to this patient? What is the natural history of this condition? Do I even need to intervene? All of these questions based around prognosis tend to receive far less attention and emphasis within physical therapy education.
Students may not even realize this is the case until they go out on clinical rotations and find themselves unprepared to answer some of these prognostic type questions. I myself am one of these students. It’s much easier to feel confident and prepared when you are in a lab with other classmates, and you are discussing fictional patient cases. Once an actual patient is sitting across from you, asking you questions and hoping for answers, the façade of certainty may disappear.
What is ‘natural history’?
Natural history refers to, “the progression of a disease process in an individual over time, in the absence of treatment.” In other words, if this patient does not receive any type of treatment or intervention, what is the probability of their diagnosis resolving on its own? And, on average, how long will this take? If there is a highly favorable natural history of a condition, such as acute non-specific low back pain, is it absolutely necessary for this patient to continue to work with me? Will additional treatment provide benefit for this condition or are we at risk of overuse of musculoskeletal (MSK) health care?
Understanding the expected course of common MSK conditions and injuries creates a great foundation when starting clinical rotations as a student. I wanted to create a resource both for myself and for other students that can be a centralized location to find the natural history and prognosis of most MSK conditions. This way, when we have a new patient on our caseload, we have a better awareness of what average recovery timelines may look like, which treatments may or may not be indicated, and what expectations to set with patients moving forward. This is by no means a comprehensive document and resource; however, I do think it is a good starting point for students to begin diving into the literature to find a specific condition’s natural history and prognosis. I have accumulated these papers over the past few years and utilize this document during my own clinical rotations. Topics include: lower back pain (LBP), Neck Pain, Elbow Tendinopathy, Ankle Sprains, Hamstring Strains, Patellofemoral Pain, and numerous other injuries. This is an evolving document that I continue to update when I find new research on a particular condition.
How to utilize this document
Step 1: Find which condition/diagnosis you are looking for.
Step 2: Read through the quotes of the papers to gain a rough understanding on the natural history and prognosis.
Step 3: Click on the hyperlink of each specific paper to gain a deeper understanding on the topic.
Step 4: Reflect and ask yourself these questions: If this condition has a favorable natural history, how do I communicate this with the patient in front of me? How much therapy (if any) do I need to provide? If this condition does not have a favorable natural history, how do I communicate this with the patient in front of me? How should I set realistic expectations on the recovery timeline? What interventions (if any) are efficacious for this condition?
Step 5: Seek out other resources and stay open minded. Again, this is by no means a complete document and it’s ultimately up to all of us, as students and future health care providers, to continue to examine the literature and update our beliefs and practices as new evidence emerges.
Here’s a couple of examples from the document
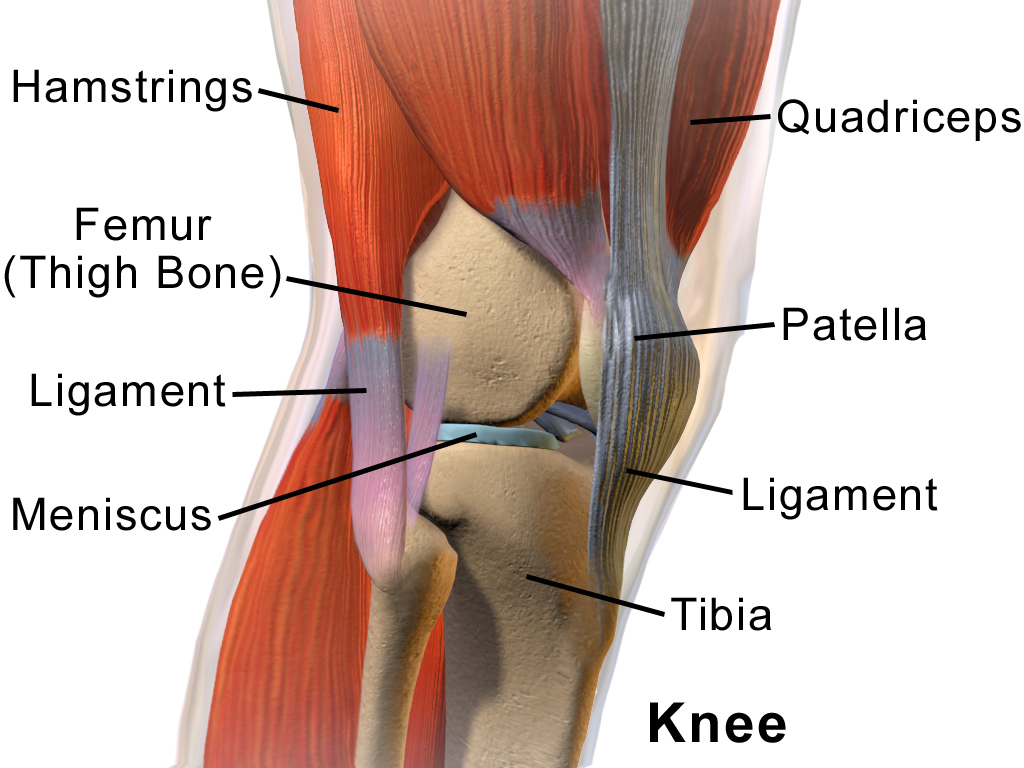
Non-Specific Acute Low Back Pain (LBP): Once you have ruled out any major red flags through a thorough subjective and objective exam, you are able to communicate the favorable natural history of acute LBP and note that a large majority of patients will improve within the first few weeks or months, regardless of different treatment types or no treatment at all. You may provide reassurance and explain what interventions are not warranted at the moment and discuss self-management strategies including routine exercise (such as individual exercise or group classes). For patients with previous history of low back pain, you may discuss the tendency of recurrence with other periods of no pain or exacerbation.
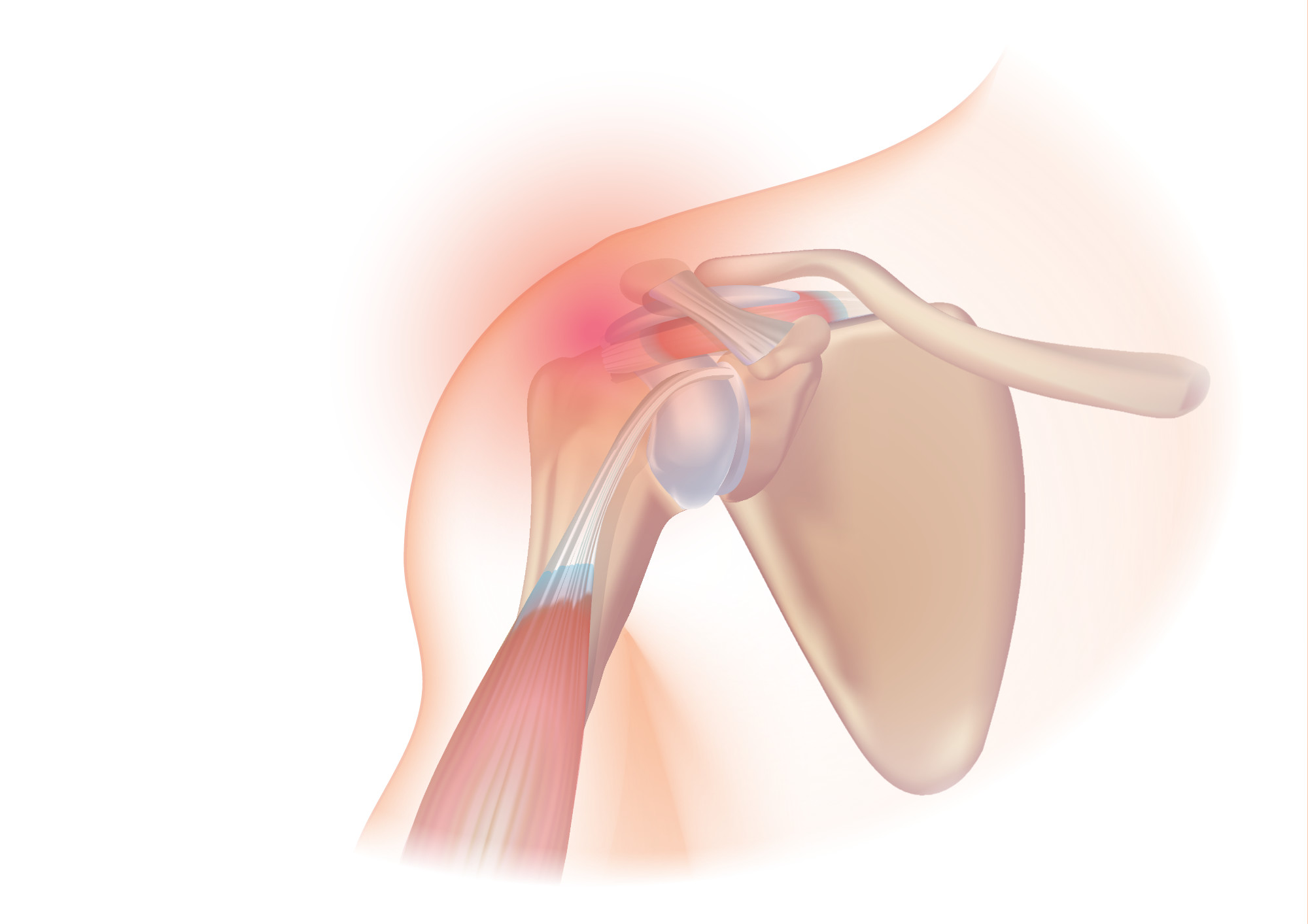
Adhesive Capsulitis / Frozen Shoulder: On the other end of the prognosis spectrum, you have adhesive capsulitis. Although this is often recognized as a self-limiting condition, that resolves spontaneously over time, there is a wide spectrum of recovery timelines, ranging from anywhere between 6-12 months all the way up to 20 years. Understanding these timelines should help guide your education with a patient diagnosed with frozen shoulder. Setting expectations that, on average, this is a much longer process than most people assume and there is quite a bit of uncertainty on how to accelerate the recovery process.
Conclusions
Understanding the natural history and average prognosis of a condition will help guide expectations for both you as a student (and future clinician) and your patients. It should direct our decision-making process on how much care is necessary versus how much a patient may improve on their own. While much attention is paid to diagnosis within the MSK rehabilitation curriculum, I wanted to shed light on the impact that prognosis will have on our communication, plan of care, and overall amount/type of intervention with each patient.
I hope some of you find this document helpful and I would love to receive feedback, either through the comment section below or by sending me an email (chrishughen1@gmail.com), on this resource and any links to research and specific conditions I have yet to cover. If you have more questions about prognostic studies or you are interested in conducting prognosis research, Cochrane published a great module covering this topic.