Making health decisions: my health deserves more
Posted on 23rd March 2023 by Hebatullah Abdulazeem

In the course of an average human lifespan of 73 years (according to WHO in 2019) many choices must be made that can affect your life. When these decisions concern your health, quality of life, and social perception and integration, it becomes imperative to carefully consider your thoughts and approach.
In this blog post, we will delve into the topic of health decision making, examining the process through the lens of two videos : “Making health decisions: what’s best for you?“– “A life-changing health decision: Sarah’s story”. These videos feature a panel of inspiring individuals, Sarah Chapman, Emma Doble, Brian Devlin, and Heather Still, who discuss real-life healthcare situations and the steps they took, or will take, to make informed health decisions. These resources, summarised in this blog, will provide support to others who are undergoing a difficult journey in determining the best course of action for their health care. Over the course of nearly 60 minutes, the panel covered three key topics: Evidence-Based Medicine (EBM), Living in reality, and a recipe for better health decision making.
Evidence-Based Medicine (EBM)
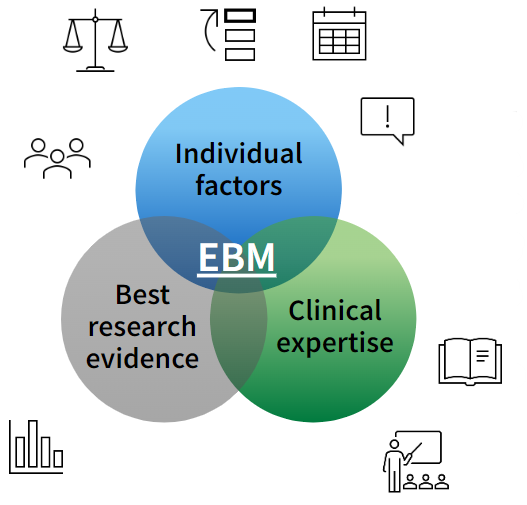
The process of making health decisions requires a strategic thinking technique that combines evidence, clinical practice, and patient preferences to reach the best possible outcome. Rebecca Gould provides an explanation of the Venn diagram triad of EBM, which consists of:
- Best Research Evidence: This refers to the authentic high-quality medical research globally produced to identify and mange health conditions
- Clinical Expertise: This item represents the medical practice and procedures performed by health care professionals in hospitals and clinics, based on available resources and guidelines
- Individual Factors: This refers to individuals’ values and what they consider to be important, as well as their own responsibility for the outcomes of their decision
Therefore, the intersection between these three elements represents the best possible health decision for each person.
Living in reality
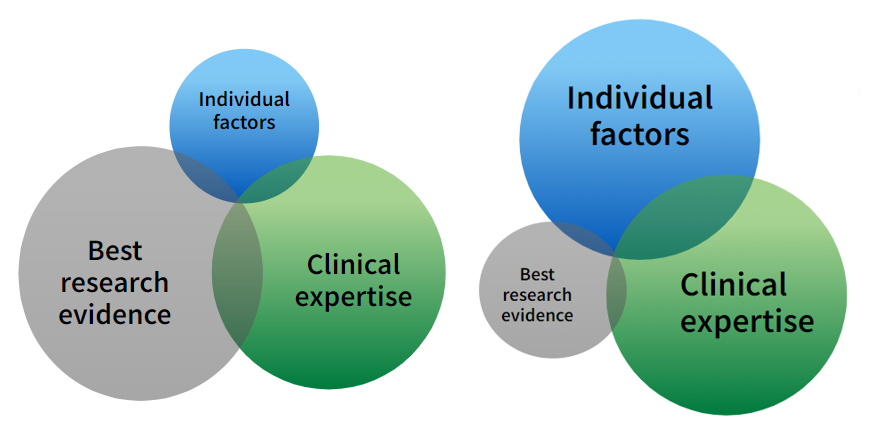
However, living exposes many challenges that we must face and hopefully overcome. We cannot deny the shortage of medical literature for some ethnic groups and rare diseases, for example. Additionally, there is the vulnerability of healthcare professionals and the sensitive situations to confront and inform patients with some sad truths. Nevertheless, the individual values of patients might not be perfectly met.
However, these interesting pieces of video were good evidence for real stories of people, with or without medical knowledge, going through this process to work hand in hand with their healthcare professionals to reach the ultimate health decision. Each member of the panel challenged a different limitation of the EBM model; nonetheless, they all manage to reach a more effective conclusion than that which emerges when only one point of view feeds into the health decision making process.
Recipe for better health decision making
This fruitful panel discussion provided us with a recipe for a better health decision-making process:
- Think “BRAIN”: this acronym refers to the assessment of Benefit, Risk, Alternatives, and Individual factors, or thinking about “Doing Nothing”. This method helps elaborate on your thoughts to balance the pros and cons of your decision
- Balance your hope with your rational self
- Take enough time to think
- Join similar communities, so you can know more and find more support
- Create an advocacy, if you cannot find any, and start supporting others along with yourself
- Try to maintain your choices that allow you to feel like yourself again
- Participate in the relevant knowledge translation for learning more about the evidence and spreading that knowledge among the public
- Figure out the questions you want to ask to help inform yourself properly before a final decision
- For you as a clinician:
- Take the chance to reassess your professional shared decision-making practice
- Provide your patients with understandable honest communication
- Give patients the chance to effectively participate in the health decision-making process
- Deliver tailored mental health input for each individual
In the end, every initiative that supports health education and evidence-based health decision making is considered as a light at the end of the illness tunnel. More community support and further high-quality research is needed.
References
Making health decisions: what’s best for you? – A 1 hour recorded webinar (20th October 2022)
A life-changing health decision: Sarah’s story – A 10-minute video which is also included in the above webinar (20th October 2022)
You may also be interested in reading the follow-up blog to the webinar – “Making health decisions: things that can help” where Sarah Chapman, Knowledge Broker at Cochrane UK, pulls together some key things that can help people make health decisions, including lots of great resources you can refer to.